Monday, August 31st, 2020
COVID-19 is deadlier than flu or H1N1 pandemic
By Leslie Gartrell
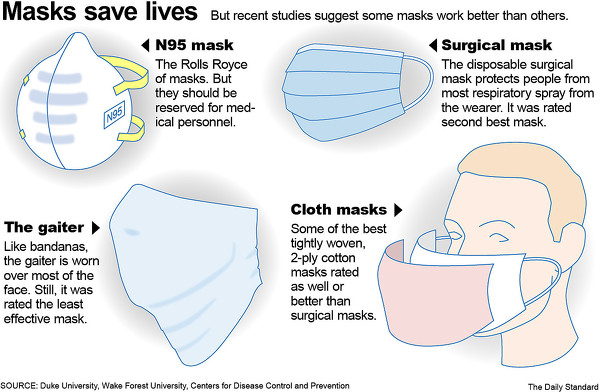
Photo by Daily Standard Staff
But recent studies suggest some masks work better than others.
Editors note: This story is the second in a series answering common questions about COVID-19 from readers and residents.
Deb Scheer, epidemiologist for both the Mercer County Health District and Auglaize County Health Department, spoke with the newspaper recently to explain some key facts on the novel coronavirus, commonly used COVID-19 terminology and why they matter. Scheer has worked in public health for more than 27 years, with a focus on infectious disease for the majority of her career.
What makes the COVID-19
pandemic different from the H1N1 flu outbreak of 2009?
In the spring of 2009, a novel influenza A (H1N1) virus emerged, according to the Centers for Disease Control and Prevention. It was detected first in the United States and spread quickly across the United States and the world, leading to a flu pandemic. This new H1N1 virus contained a unique combination of influenza genes not previously identified in animals or people.
From April 12, 2009, to April 10, 2010, the CDC estimates 60.8 million cases were reported in the U.S. and 12,469 Americans died from H1N1. Comparatively, since the beginning of the COVID-19 pandemic in the U.S. in March, 5,934,824 cases have been reported and 182,149 people have died as of Sunday, according to the CDC.
COVID-19 has proven to be more deadly than the seasonal flu and H1N1, Scheer noted, leading to an increasing sense of urgency to stop the spread of the virus.
Scheer said the COVID-19 pandemic is treated differently than the H1N1 pandemic because public health officials over time have gained more experience, knowledge and preparedness to fight a future pandemic.
Perhaps most notably, the CDC in 2017 published pre-pandemic planning guidelines based on lessons learned from the 2009 H1N1 pandemic.
The 2017 guidelines summarize key lessons learned from the H1N1 pandemic response: encourage state and local public health officials to plan and prepare for implementing non-pharmaceutical interventions early in a pandemic in community settings, describe new or updated pandemic planning and assessment tools and provide the latest scientific findings to support updated recommendations on the use of non-pharmaceutical interventions to help slow the spread and decrease the impact of a pandemic.
When a pandemic such as the H1N1 in 2009 emerges, or like the COVID-19 pandemic now, vaccines may not be available for six months or longer, and antiviral medications may be reserved for treatment and be in short supply due to high demand.
Until a vaccine or treatment is made, the CDC says non-pharmaceutical interventions delay the spread of the disease and reduce the impact of a pandemic in U.S. communities. Non-pharmaceutical interventions include actions other than use of vaccines and medications that people and communities can take to help slow the spread of a pandemic virus.
Scheer said that advice is being implemented now in the form of encouraging people to wear masks and facial coverings; practicing social distancing; limiting mass gatherings; and closing schools, places of worship and businesses.
In essence, public health officials know more now than they did in 2009, which is why mitigation efforts and non-pharmaceutical interventions such as mask wearing and social distancing is being advised now when it wasn't during the H1N1 pandemic.
Why is it important to wear a face mask or facial covering?
The CDC recommends that everyone in the U.S. wear nonsurgical masks when going out in public. COVID-19 primarily spreads when someone breathes in droplets containing virus that are produced when an infected person coughs, sneezes or talks or when a person touches a contaminated surface and then touches his or her eyes, nose or mouth.
People who are infected but do not have symptoms or have not yet developed symptoms, can also infect others. People who are infected can spread the disease 48 hours before symptoms appear. That's where masks come in.
People infected with COVID-19, even those with very mild or no symptoms, may emit aerosols when they talk or breathe. According to an online report from the Harvard Medical School, aerosols are infectious viral particles that can float or drift around in the air. Another person can breathe in these aerosols and become infected with the virus. A mask can help prevent that spread.
The CDC says masks are recommended as a simple barrier to help prevent respiratory droplets from traveling into the air and onto other people when the person wearing the mask coughs, sneezes, talks or raises his or her voice.
The use of masks is particularly important in settings where people are close to each other or unable to practice social distancing. In a study published in March in the New England Journal of Medicine, researchers found that aerosolized coronavirus could remain in the air for up to three hours.
However, the CDC has recognized that wearing masks may not be possible in every situation or for some people. Some people, such as people with intellectual and developmental disabilities, mental health conditions or other sensory sensitivities, may have challenges wearing a mask. The CDC recommends consulting with a health care provider for advice about facial coverings for people who have a disability or care for someone who does.
What kind of masks or facial coverings are most and least effective?
No matter the material or type, a facial covering should always be tight fitting and cover the nose and mouth.
Researchers at Duke University studied the effectiveness 14 different types of face masks and coverings by counting the number of droplet particles released when people spoke the phrase "stay healthy, people" five times in a row. Study participants spoke without a mask and then repeated the same phrase, each time wearing one of the 14 different types of facial coverings.
The medical-grade N95 mask performed best, meaning it had the fewest number of droplets escape. However, N95 masks are in short supply and should be reserved for health care workers.
Surgical masks followed behind N95 masks in effectiveness. Cotton masks, which many people have been making at home, also performed well. Neck gaiters, or neck fleeces, ranked dead last in effectiveness.
"We noticed that speaking through some masks (particularly the neck fleece) seemed to disperse the largest droplets into a multitude of smaller droplets, which explains the apparent increase in droplet count relative to no mask in that case," researchers wrote. "Considering that smaller particles are airborne longer than large droplets (larger droplets sink faster), the use of such a mask might be counterproductive."
The CDC does not recommend using masks that have exhalation valves or vents. Masks with one-way valves allow air to be exhaled through a hole in the material, which can result in expelled respiratory droplets that can reach others. This type of mask won't prevent a person from transmitting COVID-19 to others, according to the CDC.


